Chest pain and discomfort can frequently be attributed to digestive issues, rather than cardiac problems. Non-cardiac chest pain is the medical term for chest pain that does not originate from the heart. Conditions such as acid reflux can generate a sharp, agonizing sensation in the chest. If you experience symptoms such as shortness of breath or chest tightness, it is important to seek emergency medical assistance.
Our gastroenterologist possesses the expertise necessary to identify whether your chest pain or discomfort is due to digestive issues.
Related Symptoms
- Abdominal pain
- Acid reflux (heartburn) and indigestion
- Belching and Burping
- Hoarseness of voice
- Swallowing Problems
Is your chest pain an emergency?
Seek immediate medical advice for the following symptoms:
- Tightness in the chest
- Shortness of breath
- Pain that spreads and doesn’t go away after a few minutes
These are signs of a heart attack and require immediate assistance. If you experience these symptoms, call 999 or go to the nearest emergency room.
Chest pain symptoms caused by digestive problems
While it isn’t always clear what is causing your chest pain and discomfort, some key signs would indicate your pain is due to a digestive problem rather than a heart problem.
Signs include:
- Chest pain after eating
- Pain in your chest while you eat
- Accompanied with digestive symptoms
If you experience the following digestive symptoms alongside your chest pain, it suggests your pain is due to a digestive problem. Though, you should discuss your symptoms with a doctor to rule out other causes of your chest pain first.
Symptoms that could indicate digestive problems include :
- Hiccups
- Abdominal pain
- Constipation
- Nausea and vomiting
- Belching and burping
- Hoarseness of voice
- Swallowing problems
- Acid reflux (a burning sensation in your chest)
- Blood in your stools, stools may be dark or black
Causes of non-cardiac chest pain and discomfort :
Acid reflux, heartburn and indigestion
Acid reflux often causes a burning sensation in your chest, known as heartburn. You may also experience an unpleasant taste in your mouth. Individuals with indigestion (dyspepsia) will often feel uncomfortably full after eating and may feel sick (nausea) and bloated.
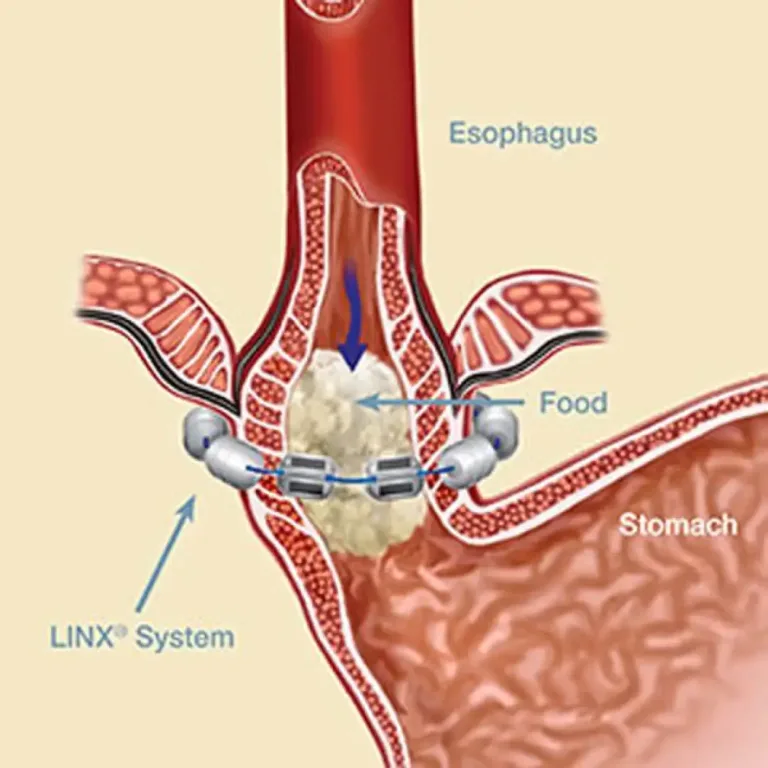
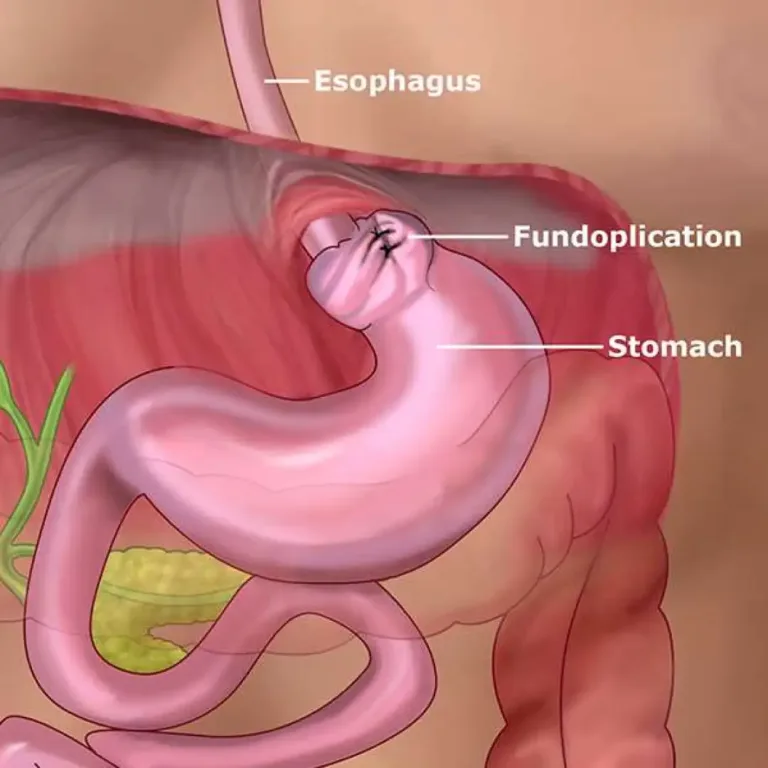
Gastro-oesophageal reflux disease
Gastro-oesophageal reflux disease (GORD) refers to excessive acid reflux. Acid and bile flow up from the stomach via the food pipe (oesophagus) due to a relaxed or weak sphincter. Left untreated, this can lead to Barrett’s oesophagus, which has similar symptoms to acid reflux. GORD is the most common reason for non-cardiac chest pain.
Irritable bowel syndrome (IBS)
IBS usually causes abdominal pain, though it may also cause pain in your chest, back, and jaw. For people with IBS, trapped gas often causes chest pain.
Functional dyspepsia
Functional dyspepsia is a medical condition characterized by persistent symptoms of indigestion without a clear underlying cause. Symptoms of functional dyspepsia may include a burning sensation in the lower chest, bloating, nausea, and belching.
Swallowing disorders
Swallowing disorders are medical conditions that affect the food pipe or oesophagus, resulting in difficulty swallowing. Pain along the oesophagus, which can be felt in the chest and other areas, may also be experienced. Such conditions may include achalasia or oesophageal spasm.
Additional digestive conditions that can cause non-cardiac chest pain
Below we list other conditions that cause chest pain and discomfort and where you are likely to feel that pain.
- Acute cholecystitis (Gallbladder inflammation) – upper chest pain on the right side
- Other gallbladder problems – possibly lower or upper chest pain on the right side
- Oesophageal hypersensitivity – higher chest pain coming from the throat area
- Oesophageal rupture – sudden, severe chest pain*
- Large hiatal hernia – lower chest pain
- Peptic ulcers – recurring discomfort
- Pancreatitis – lower chest pain
When to speak to a gastroenterologist :
After a cardiac condition has been excluded by your physician, alternative causes may be explored. If additional gastrointestinal symptoms, such as those aforementioned, are present, it would be prudent to consult with a gastroenterologist.
Our team of gastroenterologists will request a comprehensive account of your symptoms, their duration, and degree of severity. Moreover, we will delve into your medical history and that of your immediate family to deduce the most plausible causes.
Diagnosing non-cardiac chest pain
Primarily, it is imperative to establish the underlying cause of the discomfort before determining an appropriate treatment course. We can administer a variety of examinations to diagnose the source of the pain, such as an endoscopic investigation to scrutinize your oesophagus and upper gastrointestinal (GI) system.
Furthermore, other evaluations that may be conducted include:
- Barium swallow
- Laryngoscopy – If the pain extends to your throat
- Video fluoroscopy – If you are also experiencing trouble swallowing
Treatment
For a multitude of conditions that elicit thoracic pain and discomfort, we generally initiate lifestyle modifications to gauge the impact on your symptoms.
If there is an improvement in your symptoms, we may opt for monitoring your condition. Conversely, if no alteration or exacerbation is observed, pharmaceutical intervention may be prescribed. In cases of acute symptoms, alternative treatments may be recommended, contingent on the underlying cause of the condition.