Private Gastroenterology Consultations
Procedures
Private Consultations
Private Gastroenterology Consultation: What to Expect
Gastrointestinal problems can be a source of discomfort and anxiety for many people. In the UK, the National Health Service (NHS) offers excellent care, but waiting times for gastroenterology appointments can be long. If you are experiencing symptoms that are impacting your quality of life, a private gastroenterology consultation may be a good option. In this article, we will discuss what you can expect from a private gastroenterology consultation, including new consultation, follow-up consultation, and second opinion consultation.
New Consultation
If this is your first time seeing a gastroenterologist, you will likely schedule a new consultation. During this appointment, you will meet with the gastroenterologist who will review your medical history and ask you questions about your symptoms. Be prepared to provide detailed information about your symptoms, including when they started, how often they occur, and whether there are any triggers. The gastroenterologist may also ask about your family history and any previous medical procedures you have undergone.
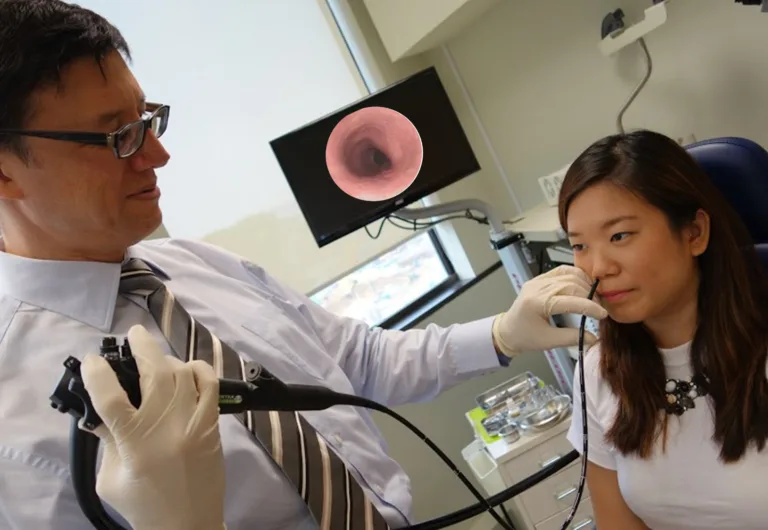
After discussing your symptoms, the gastroenterologist may perform a physical examination. Depending on your symptoms, you may need additional testing, such as blood tests, stool tests, imaging tests, or endoscopic procedures. The gastroenterologist will explain the testing process to you and answer any questions you may have.
Follow-Up Consultation
If you have already been diagnosed with a gastrointestinal condition, you may schedule a follow-up consultation with your gastroenterologist. During this appointment, the gastroenterologist will review your medical history, ask about any changes in your symptoms, and perform a physical examination. If you have undergone testing or procedures since your last appointment, the gastroenterologist will review the results with you and discuss any necessary treatment options.
If you are undergoing treatment for a gastrointestinal condition, the gastroenterologist may adjust your medication or treatment plan based on your current symptoms or test results. They will also monitor your progress and schedule any necessary follow-up appointments.
Second Opinion Consultation
If you have been diagnosed with a gastrointestinal condition but are unsure about the recommended treatment plan, you may schedule a second opinion consultation with a different gastroenterologist. During this appointment, the gastroenterologist will review your medical history, ask about your symptoms, and review any previous testing or procedures. They may perform a physical examination and order additional testing if necessary.
After reviewing your medical history and test results, the gastroenterologist will provide their opinion on your diagnosis and treatment options. They may offer alternative treatment options or suggest further testing to confirm the diagnosis. It is important to remember that a second opinion does not necessarily mean that the first gastroenterologist was incorrect. It is simply a way to ensure that you are receiving the best possible care for your condition.
In Conclusion
A private gastroenterology consultation can provide you with the care and attention you need to address your gastrointestinal symptoms. Whether you are scheduling a new consultation, a follow-up consultation, or a second opinion consultation, be prepared to provide detailed information about your symptoms and medical history. The gastroenterologist will work with you to develop a personalized treatment plan and monitor your progress to ensure that you are receiving the best possible care.
Dietitian Consultation: A Guide to Eating Well
Eating a balanced and nutritious diet is essential for maintaining good health and preventing chronic diseases. However, with so much conflicting information about what to eat and what to avoid, it can be challenging to know where to start. A dietitian consultation can help you navigate the world of nutrition and develop a personalised eating plan that works for you.
What is a Dietitian?
A dietitian is a qualified healthcare professional who specialises in the science of nutrition and dietetics. They use their knowledge of food and nutrition to help individuals achieve their health goals, whether that’s losing weight, managing a medical condition, or improving overall health and wellbeing.
What Happens During a Dietitian Consultation?
A dietitian consultation typically starts with a thorough assessment of your current health status, medical history, and dietary habits. The dietitian will ask you questions about your lifestyle, preferences, and any specific dietary needs or restrictions.
Based on this information, the dietitian will work with you to develop a personalised eating plan that meets your nutritional needs and supports your health goals. This may involve making changes to your current diet, such as increasing your intake of certain nutrients, reducing your intake of saturated fats or sugar, or incorporating more plant-based foods into your meals.
The dietitian will provide practical advice on meal planning, food preparation, and portion control, as well as tips for eating out and grocery shopping. They may also recommend specific supplements or functional foods that can support your health and wellbeing.
New Consultation
If you are seeing a dietitian for the first time, you will typically have a new consultation. This appointment usually lasts between 60 and 90 minutes and involves a comprehensive assessment of your nutritional status and health goals. The dietitian will provide you with personalised advice and a detailed eating plan to help you achieve your goals.
Follow-up Consultation
If you have already had a new consultation with a dietitian, you may require follow-up consultations to monitor your progress and make any necessary adjustments to your eating plan. Follow-up consultations can be scheduled weekly, fortnightly, or monthly, depending on your needs.
Second Opinion Consultation
If you have already received advice from a healthcare professional but would like a second opinion from a dietitian, you can book a second opinion consultation. During this appointment, the dietitian will review your medical history, dietary habits, and health goals and provide you with an alternative perspective and advice.
Benefits of Seeing a Dietitian
Seeing a dietitian can have numerous benefits for your health and wellbeing, including:
- Improved nutrition and dietary habits
- Better management of medical conditions, such as diabetes, high blood pressure, or food allergies
- Weight loss or weight gain, depending on your health goals
- Increased energy and vitality
- Enhanced sports performance
- Improved mental health and wellbeing
Conclusion
A dietitian consultation is an essential tool for anyone looking to improve their nutrition and achieve their health goals. With personalised advice and a tailored eating plan, a dietitian can help you make sustainable changes to your dietary habits and improve your overall health and wellbeing. If you are considering seeing a dietitian, speak to your healthcare provider or book an appointment with a registered dietitian today.
Gut-Directed Hypnotherapy
Gut-directed hypnotherapy is a type of therapy that aims to help individuals who suffer from functional gastrointestinal disorders (FGID). FGID is a condition that affects the digestive system and can cause a range of symptoms, such as abdominal pain, bloating, constipation, and diarrhoea. Gut-directed hypnotherapy uses hypnosis to help alleviate these symptoms and improve the quality of life for those affected by FGID.
During a gut-directed hypnotherapy session, the therapist guides the patient into a state of relaxation and uses hypnosis to help them access the subconscious mind. The therapist then uses specific suggestions to help the patient reframe their thoughts and feelings about their digestive symptoms. The aim is to help the patient learn how to better manage their symptoms by addressing the underlying psychological factors that may be contributing to their condition.
Research has shown that gut-directed hypnotherapy can be an effective treatment for FGID. A review of 35 studies found that gut-directed hypnotherapy was significantly more effective than standard medical treatments for the management of irritable bowel syndrome (IBS), which is a common FGID. In addition, gut-directed hypnotherapy has been shown to improve symptoms such as abdominal pain, bloating, diarrhoea, and constipation.
Gut-directed hypnotherapy is a safe and non-invasive treatment option for FGID. It can be particularly helpful for patients who have not found relief from traditional medical treatments. It is important to note that gut-directed hypnotherapy is not a cure for FGID, but rather a way to manage symptoms and improve quality of life.
If you are interested in gut-directed hypnotherapy, it is important to find a qualified therapist who has experience working with FGID. The therapist should be a registered practitioner with a professional body, such as the British Society of Clinical Hypnosis.
In conclusion, gut-directed hypnotherapy is a type of therapy that can help individuals who suffer from functional gastrointestinal disorders. It uses hypnosis to help alleviate symptoms such as abdominal pain, bloating, constipation, and diarrhoea. Research has shown that gut-directed hypnotherapy can be an effective treatment option for FGID. If you are interested in gut-directed hypnotherapy, it is important to find a qualified therapist with experience in treating FGID.
Consultations
New – £ 300
Follow up – £200
£ 100
Gut-directed hypnotherapy
£100 -120
(per session)
Schedule an appointment
Related Articles
Private Gastroenterology Consultations Read More »